Brody A Flanagin1, Raffaele Garofalo2, Eddie Y Lo3, LeeAnne Feher1, Alessandro Castagna4, Huanying Qin1, Sumant G Krishnan1
1 The Shoulder Center, Dallas, TX 75246, Baylor Research Institute, Dallas, TX 75204, USA
2 Shoulder Service, Miulli Hospital, Acquaviva delle Fonti-BA, Italy
3 San Francisco Multispecialty Medical Group, CA, USA
4 Shoulder and Elbow Unit, IRCCS Humanitas Institute, Milano, Italy
Correspondence Address:
Brody A Flanagin
3900 Junius Street, Suite 740, Dallas, TX 75246
USA
Login to access the Email id
Source of Support: None, Conflict of Interest: None
Abstract
Purpose: Arthroscopic transosseous (TO) rotator cuff repair has recently emerged as a new option for surgical treatment of symptomatic rotator cuff tears. Limited data is available regarding outcomes using this technique. This study evaluated midterm clinical outcomes following a novel arthroscopic TO (anchorless) rotator cuff repair technique.
Materials and Methods: A consecutive series of 107 patients and 109 shoulders underwent arthroscopic TO (anchorless) rotator cuff repair for a symptomatic full-thickness tear. Pre and postoperative range of motion (ROM) was compared at an average of 11.8 months. Postoperative outcome scores were obtained at an average of 38.0 months. Statistical analysis was performed to compare pre and postoperative ROM data. Univariate analysis was performed using Student’s t-test to compare the effect of other clinical characteristics on final outcome.
Results: Statistically significant improvements were noted in forward flexion, external rotation and internal rotation (P < 0.0001). Average postoperative subjective shoulder value was 93.7, simple shoulder test 11.6, and American Shoulder and Elbow Surgeons (ASES) score 94.6. According to ASES scores, results for the 109 shoulders available for final follow-up were excellent in 95 (87.1%), good in 8 (7.3%), fair in 3 (2.8%), and poor in 3 (2.8%). There was no difference in ROM or outcome scores in patients who underwent a concomitant biceps procedure (tenodesis or tenotomy) compared with those who did not. Furthermore, there was no significant difference in outcome between patients who underwent either biceps tenodesis or tenotomy. Age, history of “injury” preceding the onset of pain, tear size, number of TO tunnels required to perform the repair, and presence of fatty infiltration did not correlate with postoperative ROM or subjective outcome measures at final follow-up. Two complications and four failures were noted.
Conclusions: Arthroscopic TO rotator cuff repair technique leads to statistically significant midterm improvement in ROM and satisfactory midterm subjective outcome scores with low complication/failure rates in patients with average medium-sized rotator cuff tears with minimal fatty infiltration. Further work is required to evaluate radiographic healing rates with this technique and to compare outcomes following suture anchor repair.
Level of Evidence: Level IV
Keywords: Arthroscopic transosseous rotator cuff repair, rotator cuff tear, shoulder arthroscopy, suture anchors
How to cite this article:
Flanagin BA, Garofalo R, Lo EY, Feher L, Castagna A, Qin H, Krishnan SG. Midterm clinical outcomes following arthroscopic transosseous rotator cuff repair. Int J Shoulder Surg 2016;10:3-9
How to cite this URL:
Flanagin BA, Garofalo R, Lo EY, Feher L, Castagna A, Qin H, Krishnan SG. Midterm clinical outcomes following arthroscopic transosseous rotator cuff repair. Int J Shoulder Surg [serial online] 2016 [cited 2017 May 31];10:3-9. Available from: http://www.internationalshoulderjournal.org/text.asp?2016/10/1/3/174511
Introduction Top
Rotator cuff tears are a common cause of debilitating shoulder pain and dysfunction. Surgical repair of painful, symptomatic rotator cuff tears that have failed appropriate nonoperative management has been shown to be an effective method of treatment to relieve pain and improve function. [1],[2] For many years, open rotator cuff repair using transosseous (TO) sutures, first described by Codman in 1911, was considered the gold standard of surgical management for full-thickness tears. [3] However, arthroscopic rotator cuff repair with the use of suture anchors has emerged as an increasingly favorable approach worldwide to repair rotator cuff tears regardless of size and/or location. While selected studies have suggested higher retear rates with arthroscopic repair of larger tears, no significant differences in retear rates, and clinical outcomes have been consistently demonstrated in the literature between these two repair techniques. [4],[5],[6]
Many different techniques for anchor-based rotator cuff repair have been described, including single-row (SR), double-row (DR), and DR TO equivalent (TOE). [7] Significant improvement in clinical outcomes has been reported using all of these techniques. [7],[8],[9],[10],[11],[12],[13] More recently, arthroscopic TO rotator cuff repair without the use of suture anchors has also been described. [14],[15],[16] There is a relative paucity of data regarding outcomes after arthroscopic TO rotator cuff repair, but early published reports have been promising and similar to anchor-based techniques. [14],[16] No comparative clinical studies currently exist evaluating outcomes after either arthroscopic anchor-based or TO rotator cuff repair. In addition, biomechanical data has been inconclusive in demonstrating a consistent difference between these techniques. [17],[18],[19],[20],[21],[22] Given the results of these studies combined with individual patient factors unique to each case (i.e., tear size, tendon/bone quality, amount of retraction, etc.,) the “ideal” or “gold standard” of arthroscopic rotator cuff repair remains unknown ). [1] .
To this end, we report midterm clinical outcomes following a novel arthroscopic TO rotator cuff repair technique. Our hypothesis was that this technique would lead to significant improvements in postoperative range of motion (ROM) and clinical outcomes.
Materials and methods Top
Between June 2009 and June 2011, we identified 131 consecutive patients and 133 shoulders (2 patients underwent bilateral rotator cuff repair during the study time frame) with a full-thickness rotator cuff tear, repairable without any tension to the native footprint who underwent arthroscopic TO rotator cuff repair by the senior author (SGK). All patients presented with a complaint of shoulder pain/dysfunction and had attempted a variety of nonopervative treatment measures including activity modification, oral anti-inflammatory medications, physical therapy, and corticosteroid injection(s) without sustained relief and elected to undergo surgical treatment. Five patients had prior surgery on the ipsilateral shoulder, and 7 patients underwent concomitant suprascapular nerve decompression and were excluded from the final analysis. Twelve patients could not be contacted via either email or telephone and were considered lost to follow-up. Complete data regarding ROM and subjective outcome scores were available from 107 to 131 (81.7%) patients and 109/133 (82%) shoulders for final analysis.
We retrospectively reviewed the charts of these patients to record objective pre and postoperative ROM. Anterior elevation and external rotation were measured with the use of a goniometer. Internal rotation was measured to the maximum vertebral level with the hand behind the back. Operative reports were reviewed to document the exact operative procedure performed including the number of a tendon(s) torn/repaired as well as the presence of chondral lesions involving the glenohumeral articular cartilage as described by Outerbridge. [23] Since our X-rays were not performed under fluoroscopic control, radiographic measurements of acromiohumeral interval, or joint space were not performed. Preoperative magnetic resonance imaging (MRI) and/or computed tomography (CT) was reviewed by a musculoskeletal radiologist and fellowship-trained shoulder to determine the amount of fatty infiltration of the torn rotator cuff tendon(s) according to the staging systems of Goutallier et al. and Fuchs et al. [24],[25] Subjective outcome scores including subjective shoulder value (SSV), simple shoulder test (SST), and American Shoulder and Elbow Surgeons (ASES) score were obtained via electronic or telephonic survey by a fellowship-trained shoulder and elbow surgeon who was not involved in the care of any patients included in this series. Of note, no preoperative subjective outcome scores were available for comparison. Patient outcomes were classified according to the postoperative ASES score as excellent (90-100), good (80-89), fair (70-79), or poor (<70). [26] Patients with a postoperative ASES score of <70 were considered failures. Statistical analysis was then performed to compare pre and postoperative ROM data. Univariate analysis was performed using Student’s t-test to compare the effect of other clinical characteristics on final outcome.
There were 59 males and 48 females with an average age of 56.3 years (range: 28-72 years) at the time of surgery. Eighty patients underwent surgery on their dominant shoulder. Thirty-nine patients reported an “injury” that preceded the onset of their pain. The average duration of symptoms prior to surgery was 47.1 months. Twenty-eight patients previously attempted physical therapy and 36 reported a history of one or more cortisone injections prior to surgery. The exact number of injections each patient had been not able to be obtained from clinical records.
Average Outerbridge staging was 1.2 (range: 0-3). Average rotator cuff tear size as evaluated arthroscopically after minimal debridement was 2.5 cm in the sagittal plane (range: 1-6 cm) by 1.8 cm in the coronal plane (range: 1-4 cm). Tear pattern was as follows: 21 supraspinatus; 82 supraspinatus and infraspinatus; 3 subscapularis; 2 subscapularis and supraspinatus; and 1 subscapularis, supraspinatus, and infraspinatus. Average preoperative Goutallier et al. classification was 0.7 for supraspinatus tears (range: 0-3), 0.8 for infraspinatus tears (range: 0-2), and 1.3 for subscapularis tears (range: 0-3). An average of 1.8 TO tunnels were used to perform the cuff repair (range: 1-4). A simple suture configuration was utilized in all 40 patients with a one tunnel repair; XBOX suture configuration was incorporated in 17 patients with a two tunnel repair; mattress configuration was used in all remaining patients regardless of the number of TO tunnels [Figure 1]. Patients who underwent either biceps tenotomy or tenodesis were included for analysis. Ten patients had a biceps tenotomy, and 40 patients underwent biceps tenodesis at the time of surgery. Biceps tenodesis was performed in 15/40 patients with suprapectoral interference screw fixation and in 25/40 via TO sutures incorporated into the cuff repair. Summary of demographic, clinical, and radiographic characteristics is listed in [Table 1].
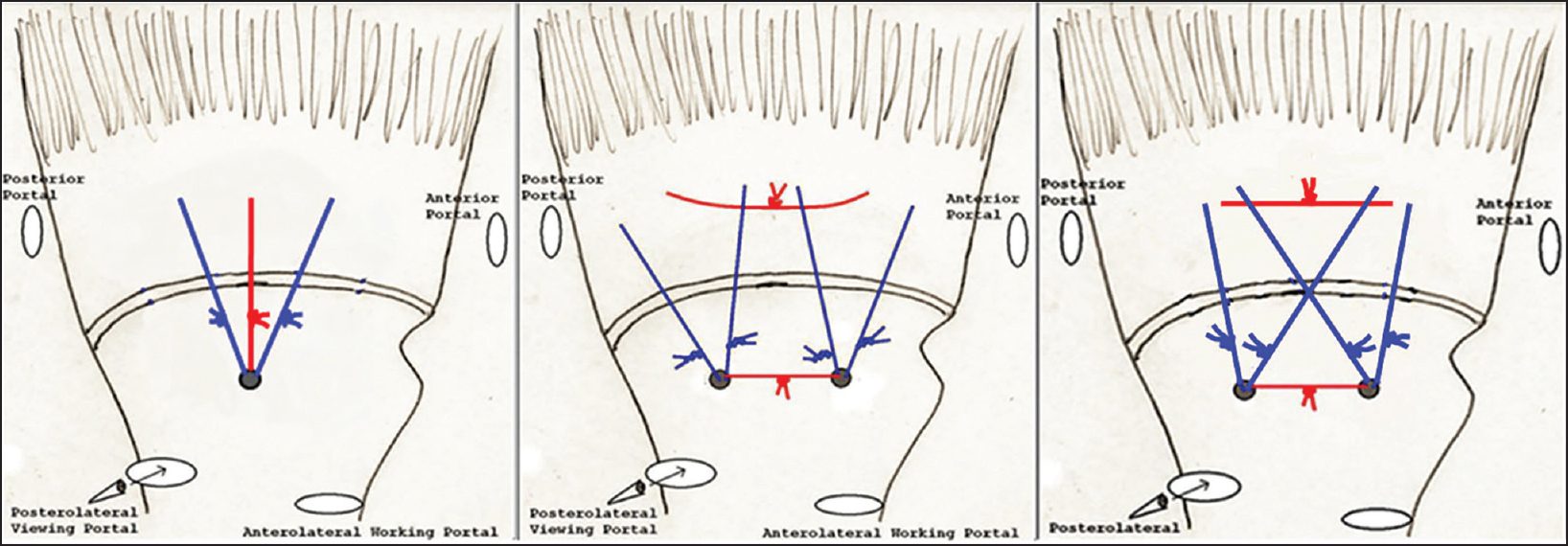 |
Figure 1: Arthroscopic pictures of one tunnel simple (left), two tunnel mattress (middle), and two tunnel XBOX (right) repair configurations
Click here to view |
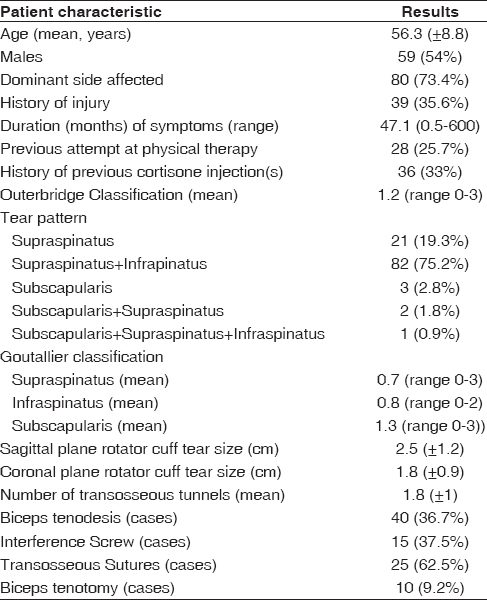 |
Table 1: Summary of demographic, clinical, and radiographic characteristics Mean (standard deviation) is listed for continuous variables and n (%) for categorical variables Click here to view |
This study was approved by the Institutional Review Board of the Baylor Research Institute, an affiliate of the Baylor Health Care system (No. 013-123). All patients gave individual informed consent to participate in the study. No outside financial support was utilized to complete this study.
Surgical technique
All surgery was performed under general anesthesia in a modified beach chair position with the patient’s back nearly vertical (“dinner chair position”). No peripheral nerve blocks were utilized either pre or postoperatively in any patient. A four portal (anterior, posterior, anterolateral, and postero-lateral) technique was utilized in all cases. In patients who underwent biceps tenodesis with an interference screw, a fifth portal was added approximately 2 cm distal to the anterolateral corner of the acromion in line with the biceps tendon/transverse humeral ligament.
Routine diagnostic arthroscopy was followed by subacromial decompression/bursectomy with a limited acromioplasty of the anterolateral corner of the acromion preserving coracoacromial ligament in all patients. If proximal disinsertion, fraying/tearing, instability, or tenosynovitis of the biceps tendon was visualized, a tenotomy at the supraglenoid tubercle was performed during diagnostic arthroscopy. Biceps tenodesis was performed in younger, active patients, or in those patients who expressed concern about cosmetic deformity (i.e., “Popeye” sign) or cramping associated with tenotomy alone. If a tenodesis was performed, it was carried out either by suprapectoral tenodesis 1 cm below the top of the bicipital groove with an interference screw or (2) TO sutures using a lasso loop technique incorporated into the rotator cuff repair. Arthroscopic distal clavicle resection was performed in 31 patients in this series after rotator cuff repair was complete. All these patients had preoperative tenderness to palpation at the acromioclavicular joint with concomitant degenerative changes noted on preoperative imaging (X-ray, MRI, and/or CT scan).
All patients underwent arthroscopic TO rotator cuff repair for superior and/or postero-superior lesions as previously described by Garofalo et al. [15] For subscapularis repair, these lesions were repaired from the subacromial space using the same technique with slight modifications as deemed necessary for the introduction of instrumentation/suture management/suture tying. No suture anchors were utilized in any case. After subacromial decompression, footprint preparation and appropriate releases of the rotator cuff, intersecting TO bone tunnels were created using the ArthroTunneler™ (Tornier, Edina, MN, USA) technique. The number of tunnels was determined at the time of surgery based on the tear size/number of tendons torn. In general, we utilize one TO tunnel per centimeter of tearing in the sagittal plane. The size of the tear in the coronal plane (i.e., amount of retraction) does not typically influence the number of tunnels utilized for the repair. Our preference is to shuttle three high-tensile strength sutures through each tunnel: Two #2 Orthocord ® (Ethicon, Somerville, NJ, USA) semi-permanent sutures and one #3-4 Force Fiber™ (Tornier, Edina, MN, USA) permanent suture. The sutures were passed through the rotator cuff using a combination of antegrade/retrograde delivery technique, retrieved and tied in either a simple, XBOX or mattress configuration [Figure 2]. Of note, advanced repair techniques such as side-to-side sutures for L-shaped/reverse L-shaped tears and margin convergence techniques for larger U-shaped tears were utilized in 35/109 shoulders. However, with careful attention to the utilization of appropriate arthroscopic releases and advanced repair techniques when needed all tears were able to mobilize and repair to their native footprint. No bone augmentation device was utilized in any patient in this series.
| Figure 2: Schematic drawings of one tunnel simple (left), two tunnel mattress (middle), and two tunnel XBOX (right) repair configurations
Click here to view |
Postoperative care and rehabilitation
Postoperatively, all patients were placed into a simple arm sling (SmartSling ® , Ossur Medical, Pauling Ranch, CA, USA) with the arm at the side and an additional strap around the waist for 6 weeks. No abduction pillows were used for any patient regardless of tear size. Immediate passive and active assisted elbow/wrist/hand motion and scapular kinetic exercises were started the day after surgery. Supervised physical therapy was initiated within the first 7-10 days after surgery. We begin immediate supine passive anterior elevation and external rotation for the first 6 weeks and advance accordingly during this time based on the size of the tear. Active ROM (including initiation of internal rotation) was started at week seven out of the sling and gentle strengthening typically by week 12. Full release to all activities is patient specific but is generally allowed by 6 months after surgery.
Statistical analysis
All statistical analyses were performed using SAS software version 9.3 (SAS Institute Inc., Cary, NC, USA). Paired samples t-test was used to compare pre and postoperative ROM data. Univariate analysis was performed using Student’s t-test to compare the effect of various demographic/clinical characteristics on final outcome. A P < 0.05 was considered to indicate statistical significance.
Results Top
At an average of 11.9 months, mean active anterior elevation improved by 12.2°, external rotation with the arm at side by 12.9°, and internal rotation by 2.0 vertebral levels (P < 0.0001). At an average follow-up of 38.0 months, mean SSV was 93.7 (range: 5-100), SST 11.6 (range: 1-12), and 94.6 (range: 26.7-100). According to ASES scores, results for the 109 shoulders available for final follow-up were excellent in 95 (87.1%), good in 8 (7.3%), fair in 3 (2.8%), and poor in 3 (2.8%). There was no difference in outcomes between patients who had biceps procedure (i.e., tenotomy or tenodesis) or not. Age, history of “injury” preceding the onset of pain, tear size, number of TO tunnels required to perform the repair, and presence of fatty infiltration did not correlate with postoperative ROM or subjective outcome measures at final follow-up in this cohort. No intraoperative fractures of the greater tuberosity were encountered in this series.
Two complications occurred in two shoulders resulting in repeat surgery. One patient who underwent interference screw biceps tenodesis had an atraumatic failure at 2 weeks postoperatively and underwent revision open subpectoral biceps tenodesis. Another patient had persistent drainage from the anterior portal and was taken back to the operating room at 4 weeks postoperatively for arthroscopic irrigation and debridement and treated with parenteral antibiotics for 6 weeks (intraoperative cultures were negative). According to postoperative ASES scores, both of these patients had an excellent result at final follow-up. There were four failures: One patient underwent revision rotator cuff repair 2 years after the original surgery for a recurrent tear, and three patients had postoperative ASES scores <70 at final follow-up.
Discussion Top
The primary goals of rotator cuff repair are pain relief, improvement in function and successful healing of the tendon. Gerber et al. stated “the ideal repair should have high initial strength, allow minimal gap formation and maintain stability until solid healing.” [27] Despite the availability of many different techniques to fix the rotator cuff either open or arthroscopically, the “ideal” method or “gold standard” of repair continues to remain a debated topic. The use of suture anchors is by far the most common method in which arthroscopic rotator cuff repair is currently performed. SR, DR, and TOE anchor-based repair methods are well-described in the literature and have consistently demonstrated good clinical outcomes and healing rates. [7],[8],[9],[10],[11],[12],[13] Arthroscopic TO (i.e., “anchorless”) rotator cuff repair has recently emerged as another viable option in the armamentarium of arthroscopic shoulder surgeons. [14],[15],[16] However, there are a limited number of published studies regarding clinical outcomes. [14],[16]
One series of studies demonstrated greater contact and pressure distribution with superior tendon fixation and reduced motion at the tendon-to-tuberosity interface with a simple TO repair configuration compared to anchor-based SR simple and mattress repair techniques. [17],[21] However, Mazzocca et al. have also previously shown that a TOE repair had higher contact pressure and force at all-time points during load to failure when compared to SR, DR and TO repair techniques. [20] Salata et al. demonstrated significantly higher load to failure with a TOE repair compared to three separate TO repair techniques, two of which utilized the same device and similar suture configurations as presented in this study. [22] Furthermore, other studies have shown no significant difference in fixation strength and stability between TOE and TO rotator cuff repair. [18],[19]
This study evaluated the clinical outcomes (ROM and subjective outcome scores) following a novel arthroscopic TO rotator cuff repair using a technique previously described by Garofalo et al. [15] There is currently no published clinical outcome data in the peer-reviewed literature following this repair technique. Our results demonstrated statistically significant improvements in ROM in forward flexion, external rotation, and internal rotation (P < 0.0001). At a mean follow-up of 38.0 months, average postoperative SSV was 93.7, and average SST was 11.6. According to the postoperative ASES score, 97.2% of shoulders obtained a successful result (postoperative ASES score >70). Complication (1.8%) and failure (3.7%) rates were low and not associated with the surgical technique. Furthermore, no intraoperative fractures of the greater tuberosity were encountered in this series.
There are several weaknesses relevant to this study. This study analyzed a consecutive group of patients with a very heterogeneous distribution of rotator cuff tears with respect to size/number of tendons involved, tear configuration and tear type (i.e., traumatic vs. degenerative). The inclusion of patients who underwent associated arthroscopic procedures could have served as a confounding variable. This is particularly important with respect to patients who underwent a concomitant biceps tendon procedure (tenotomy/tenodesis). Previous studies have suggested that healing of the rotator cuff tendon(s) the following repair does not necessarily correlate with clinical outcomes. [28] We do acknowledge there may exist some patients in this study with the failure of tendon healing who reported improvement and pain relief as a result of treatment of relevant biceps tendon pathology with either tenotomy or tenodesis. With respect to patients who underwent biceps tendon procedures, we reported no difference between those who underwent either tenotomy or tenodesis. Given this was a small number of patients, it is possible that this portion of the statistical analysis was underpowered to detect an actual difference in these two groups of patients. In addition, no preoperative subjective outcome scores were available in the preoperative clinical documentation and thus no comparison could be made between preoperative and postoperative subjective outcome scores. This serves as a significant weakness to the interpretation of the results; however, we feel that the high overall average postoperative SSV, SST, and ASES scores are suggestive of the potential efficacy of this technique. In addition, use of the ASES score has its inherent weaknesses as an outcomes measure and our decision to stratify outcomes according to the ASES score (i.e., excellent, good, fair, and poor) is somewhat arbitrary as well. However, we feel that providing the SSV as a marker of patient satisfaction along with the SST helps to strengthen the findings of this study and support high average final ASES scores we observed. Furthermore, postoperative MRIs were not obtained on the vast majority of this cohort during the study time frame and therefore we cannot comment on repair integrity/healing rates with this technique.
Conclusions Top
Arthroscopic TO rotator cuff repair using the ArthroTunneler™ technique leads to significant midterm improvement in ROM and satisfactory mid-term subjective outcome scores with low complication/failure rates in patients with average medium-sized rotator cuff tears with minimal fatty infiltration. This technique could be a viable option in the treatment of rotator cuff tear, but further studies need to be performed to evaluate clinical and radiographic outcomes with this technique.
Compliance with ethical standards
All procedures performed for this study were in accordance with the Ethical Standards of the Institutional and/or the National Research Committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study was approved by the Institutional Review Board of the Baylor Research Institute, an affiliate of the Baylor Health Care system (No. 013-123). Informed consent was obtained from all individual participants included in the study. Sumant Krishnan, MD, received royalties and consultant payments from Tornier and TAG Medical, which is related to the subject of this work. The remaining authors have no conflict of interest to disclose related to the subject of this article. No outside financial support was utilized to complete this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References Top
1.
Aleem AW, Brophy RH. Outcomes of rotator cuff surgery: What does the evidence tell us? Clin Sports Med 2012;31:665-74. Back to cited text no. 1
2.
Mather RC 3 rd , Koenig L, Acevedo D, Dall TM, Gallo P, Romeo A, et al. The societal and economic value of rotator cuff repair. J Bone Joint Surg Am 2013;95:1993-2000. Back to cited text no. 2
3.
Codman EA. Complete rupture of the supraspinatus tendon. Operative treatment with report of two successful cases. Boston Med Surg J 1911;164:708-10. Back to cited text no. 3
4.
Bishop J, Klepps S, Lo IK, Bird J, Gladstone JN, Flatow EL. Cuff integrity after arthroscopic versus open rotator cuff repair: A prospective study. J Shoulder Elbow Surg 2006;15:290-9. Back to cited text no. 4
5.
Lindley K, Jones GL. Outcomes of arthroscopic versus open rotator cuff repair: A systematic review of the literature. Am J Orthop (Belle Mead NJ) 2010;39:592-600. Back to cited text no. 5
6.
Van der Zwaal P, Thomassen BJ, Nieuwenhuijse MJ, Lindenburg R, Swen JW, van Arkel ER. Clinical outcome in all-arthroscopic versus mini-open rotator cuff repair in small to medium-sized tears: A randomized controlled trial in 100 patients with 1-year follow-up. Arthroscopy 2013;29:266-73. Back to cited text no. 6
7.
Dines JS, Bedi A, ElAttrache NS, Dines DM. Single-row versus double-row rotator cuff repair: Techniques and outcomes. J Am Acad Orthop Surg 2010;18:83-93. Back to cited text no. 7
8.
Boileau P, Brassart N, Watkinson DJ, Carles M, Hatzidakis AM, Krishnan SG. Arthroscopic repair of full-thickness tears of the supraspinatus: Does the tendon really heal? J Bone Joint Surg Am 2005;87:1229-40. Back to cited text no. 8
9.
Kim KC, Shin HD, Lee WY. Repair integrity and functional outcomes after arthroscopic suture-bridge rotator cuff repair. J Bone Joint Surg Am 2012;94:e48. Back to cited text no. 9
10.
Lafosse L, Brozska R, Toussaint B, Gobezie R. The outcome and structural integrity of arthroscopic rotator cuff repair with use of the double-row suture anchor technique. J Bone Joint Surg Am 2007;89:1533-41. Back to cited text no. 10
11.
Lapner PL, Sabri E, Rakhra K, McRae S, Leiter J, Bell K, et al. A multicenter randomized controlled trial comparing single-row with double-row fixation in arthroscopic rotator cuff repair. J Bone Joint Surg Am 2012;94:1249-57. Back to cited text no. 11
12.
Neyton L, Godenèche A, Nové-Josserand L, Carrillon Y, Cléchet J, Hardy MB. Arthroscopic suture-bridge repair for small to medium size supraspinatus tear: Healing rate and retear pattern. Arthroscopy 2013;29:10-7. Back to cited text no. 12
13.
Sugaya H, Maeda K, Matsuki K, Moriishi J. Repair integrity and functional outcome after arthroscopic double-row rotator cuff repair. A prospective outcome study. J Bone Joint Surg Am 2007;89:953-60. Back to cited text no. 13
14.
Baudi P, Rasia Dani E, Campochiaro G, Rebuzzi M, Serafini F, Catani F. The rotator cuff tear repair with a new arthroscopic transosseous system: The Sharc-FT (®) . Musculoskelet Surg 2013;97 (Suppl 1):57-61. Back to cited text no. 14
15.
Garofalo R, Castagna A, Borroni M, Krishnan SG. Arthroscopic transosseous (anchorless) rotator cuff repair. Knee Surg Sports Traumatol Arthrosc 2012;20:1031-5. Back to cited text no. 15
16.
Kuroda S, Ishige N, Mikasa M. Advantages of arthroscopic transosseous suture repair of the rotator cuff without the use of anchors. Clin Orthop Relat Res 2013;471:3514-22. Back to cited text no. 16
17.
Ahmad CS, Stewart AM, Izquierdo R, Bigliani LU. Tendon-bone interface motion in transosseous suture and suture anchor rotator cuff repair techniques. Am J Sports Med 2005;33:1667-71. Back to cited text no. 17
18.
Behrens SB, Bruce B, Zonno AJ, Paller D, Green A. Initial fixation strength of transosseous-equivalent suture bridge rotator cuff repair is comparable with transosseous repair. Am J Sports Med 2012;40:133-40. Back to cited text no. 18
19.
Kummer FJ, Hahn M, Day M, Meislin RJ, Jazrawi LM. A laboratory comparison of a new arthroscopic transosseous rotator cuff repair to a double row transosseous equivalent rotator cuff repair using suture anchors. Bull Hosp Jt Dis 2013;71:128-31. Back to cited text no. 19
20.
Mazzocca AD, Bollier MJ, Ciminiello AM, Obopilwe E, DeAngelis JP, Burkhart SS, et al. Biomechanical evaluation of arthroscopic rotator cuff repairs over time. Arthroscopy 2010;26:592-9. Back to cited text no. 20
21.
Park MC, Cadet ER, Levine WN, Bigliani LU, Ahmad CS. Tendon-to-bone pressure distributions at a repaired rotator cuff footprint using transosseous suture and suture anchor fixation techniques. Am J Sports Med 2005;33:1154-9. Back to cited text no. 21
22.
Salata MJ, Sherman SL, Lin EC, Sershon RA, Gupta A, Shewman E, et al. Biomechanical evaluation of transosseous rotator cuff repair: Do anchors really matter? Am J Sports Med 2013;41:283-90. Back to cited text no. 22
23.
Outerbridge RE. The etiology of chondromalacia patellae. J Bone Joint Surg Br 1961;43-B:752-7. Back to cited text no. 23
[PUBMED]
24.
Goutallier D, Postel JM, Bernageau J, Lavau L, Voisin MC. Fatty muscle degeneration in cuff ruptures. Pre- and postoperative evaluation by CT scan. Clin Orthop Relat Res 1994;304:78-83. Back to cited text no. 24
25.
Fuchs B, Weishaupt D, Zanetti M, Hodler J, Gerber C. Fatty degeneration of the muscles of the rotator cuff: Assessment by computed tomography versus magnetic resonance imaging. J Shoulder Elbow Surg 1999;8:599-605. Back to cited text no. 25
26.
Duralde XA, McClelland WB Jr. The clinical results of arthroscopic transtendinous repair of grade III partial articular-sided supraspinatus tendon tears. Arthroscopy 2012;28:160-8. Back to cited text no. 26
27.
Gerber C, Schneeberger AG, Beck M, Schlegel U. Mechanical strength of repairs of the rotator cuff. J Bone Joint Surg Br 1994;76:371-80. Back to cited text no. 27
28.
Russell RD, Knight JR, Mulligan E, Khazzam MS. Structural integrity after rotator cuff repair does not correlate with patient function and pain: A meta-analysis. J Bone Joint Surg Am 2014;96:265-71. Back to cited text no. 28
Figures
[Figure 1], [Figure 2]
Tables
