Joshua D Harris, Michael J Griesser, Grant L Jones
Department of Orthopaedics, The Ohio State University Sports Medicine Center, Columbus, Ohio, USA
Correspondence Address:
Grant L Jones
The Ohio State University Sports Medicine Center, 2050 Kenny Road, Suite 3100, Columbus – 43221, Ohio
USA
Login to access the Email id
DOI: 10.4103/0973-6042.80461
PMID: 21660192
Abstract
The optimal surgical treatment for symptomatic os acromiale that has failed nonoperative management is unclear in the literature. We conducted a systematic review of multiple medical databases for level I-IV evidence. Both radiographic and clinical outcomes were analyzed. Nine studies met the inclusion criteria (118 subjects, 125 shoulders). One hundred and fifteen subjects were treated surgically (122 shoulders). The mean age of the subjects was 49±11 years. The mean preoperative duration of symptoms was 12±8.6 months. Mesoacromiale was the most common type treated (94%). Internal fixation was the most common surgical technique used (60%), followed by excision (27%) and acromioplasty (13%). Rotator cuff repair was the most common concurrent surgical technique (performed in 59% of the surgically treated shoulders), followed by distal clavicle excision (25%). All surgical techniques resulted in improvement in clinical outcomes. Surgical management of symptomatic os acromiale that has failed nonoperative measures may predictably lead to improved outcomes.
Keywords: Acromionectomy, acromioplasty, excision, internal fixation, os acromiale
How to cite this article:
Harris JD, Griesser MJ, Jones GL. Systematic review of the surgical treatment for symptomatic os acromiale. Int J Shoulder Surg 2011;5:9-16
How to cite this URL:
Harris JD, Griesser MJ, Jones GL. Systematic review of the surgical treatment for symptomatic os acromiale. Int J Shoulder Surg [serial online] 2011 [cited 2013 Apr 19];5:9-16. Available from: http://www.internationalshoulderjournal.org/text.asp?2011/5/1/9/80461
Introduction Top
Appearance of the acromial centers of ossification (preacromion, mesoacromion, metaacromion and basiacromion) occurs between 15 and 18 years of age and should complete by 25 years of age. [1] An os acromiale is a failure of fusion at one of the junctions of these ossification centers. The incidence of the os acromiale ranges from 1% to 30%. [2] Bilateral involvement may occur in 33% [3],[4] -62% [5] of the cases. The most common nomenclature denotes naming of the os acromiale by the fragment anterior to the unfused segments (hence, an ununited mesoacromion and metaacromion is called a mesoacromiale) [Figure 1]. Thus, the bone anterior to the site of the two most anterior unfused segments is called “preacromiale.” The mesoacromiale is the most common os acromiale type, followed by preacromiale and then metaacromiale. [3],[4]
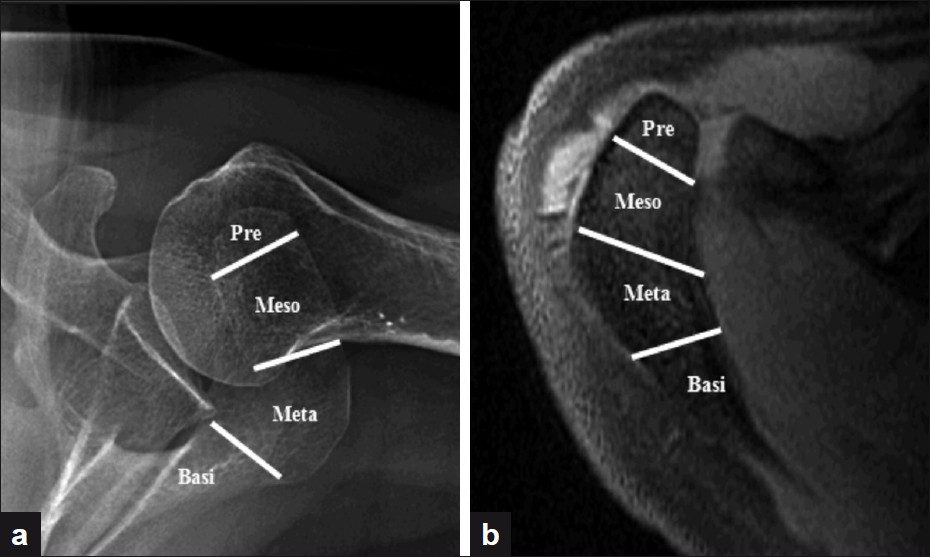 |
Figure 1: (a) Axillary radiograph; (b) Axial magnetic resonance image. (Pre – Preacromiale; Meso – Mesoacromiale; Meta – Metaacromiale; Basi – Basiacromiale)
Click here to view |
Clinical manifestations of symptomatic os acromiale involve impingement-like pain, night pain and tenderness at the site of the ununited fragments. Pathomechanisms involved include excessive motion at this ununited site, predisposing to subacromial impingement and, potentially indirectly, rotator cuff tears and also degenerative pseudarthrosis changes with cyst formation. The “false-articulation” may actually be like a true synovial joint with articular cartilage [6] or may be a fibrous synchondrosis. [7] Diagnosis of symptomatic os acromiale may preclude allowance of time in patients less than 25 years of age. Nevertheless, this diagnosis has been made in age ranges from teenagers [8] to the elderly. [9] Nonsurgical management has traditionally been the initial treatment of choice in all cases of os acromiale. [2] Failure of nonoperative measures may require surgical intervention. Surgical options include excision of the os acromiale fragment, subacromial acromioplasty and internal fixation. The high incidence of concurrent rotator cuff tear warrants consideration during rotator cuff repair. [2] Although concurrent symptomatic acromioclavicular (AC) joint osteoarthritis has been reported, [10] the AC joint is a stabilizing structure for a mesoacromiale; thus, its removal during a distal clavicle excision would further destabilize the os acromiale. In addition, given that the origin of vascularity for the anterior acromion is anteromedial, [2] a distal clavicle excision may compromise the requisite blood supply to the anterior os acromiale fragment, should fixation be attempted, increasing the risk of nonunion. Small pre os acromiale fragments generally do well with excision and meticulous deltoid repair. Large unstable meso- or meta-os acromiale fragments generally do poorly with excision/acromionectomy. The choice of fixation versus acromioplasty versus excision has yet to be demonstrated clearly in the literature for symptomatic, stable or unstable, pre-, meso- and meta-os acromiale.
The purpose of this review was to report and compare the clinical and radiographic outcomes following surgical management of symptomatic os acromiale. We hypothesized that (1) excision of pre os acromiale leads to improved clinical outcomes, (2) arthroscopic excision of meso- and meta-os acromiale fragments leads to improved clinical outcomes while open excision (without deltoid repair) leads to poor clinical outcomes, (3) arthroscopic acromioplasty of stable os acromiale leads to improved clinical outcomes and (4) stable fixation of meso- and meta-os acromiale fragments leads to improved clinical outcomes.
Methods
To address our hypotheses, we performed a systematic review of the available medical literature using several medical databases, including Pubmed, MEDLINE, CINAHL (Cumulative Index to Nursing and Allied Health Literature), SPORTDiscus with full text and Cochrane Central Register of Controlled Trials/Database of Systematic Reviews/Methodology Register. The search was independently performed by all three authors (JDH, MJG, GLJ) on August 7, 2010. Database journal search dates ranged from 1950 to the current day. Search terms included “os acromiale,” “fixation,” “excision” and “repair.” Levels I, II, III and IV evidence (according to the Oxford Centre for Evidence-Based Medicine used by the American version of the Journal of Bone and Joint Surgery) were applied. [11] Potential inclusive papers and their bibliographies were manually reviewed and discussed among authors and a decision was made regarding the inclusion or exclusion. In the event of disagreement among authors for study inclusion, the final decision was made by the senior author (GLJ). The full text article was reviewed and the reference list was checked for potential studies not identified by our original search.
Inclusion criteria
The inclusion criteria were:
Level I, II, III and IV evidence studies
English language studies
Human subjects
Study publication date from January 1, 1950 to August 7, 2010
Studies investigating clinical outcomes following treatment of symptomatic os acromiale
Studies investigating nonoperative management of symptomatic os acromiale
Studies investigating operative management of symptomatic os acromiale, including fragment excision/acromioplasty/acromionectomy and internal fixation/repair
Studies with a minimum mean follow-up of 24 months
Exclusion criteria
The exclusion criteria were:
Level V evidence studies and Level IV evidence isolated patient/subject case reports
Non-English language
Basic science, animal model, biomechanical studies
Studies not reporting clinical outcomes following treatment of symptomatic os acromiale
Studies investigating fixation or repair of iatrogenically separated (for visualization of subacromial space and rotator cuff repair) os acromiale
Studies reporting only imaging (X-ray, ultrasound, computed tomography or magnetic resonance imaging) outcomes
Studies with a mean follow-up of less than 24 months
[Table 1] displays the search strategy citation results of all databases searched. Forty-two studies were initially retained and analyzed further for potential inclusion. One study was excluded due to non-English language (Turkish). [12] Twelve Level IV isolated subject case reports were excluded. [13],[14],[15],[16],[17],[18],[19],[20],[21],[22],[23],[24]
| Table 1: Database search citation strategy
Click here to view |
Five imaging studies without clinical outcomes were excluded. [3],[25],[26],[27],[28] Two studies reported long-term outcomes following acromionectomy for multiple reasons (however, none for os acromiale) and were excluded. [29],[30] Two studies reported an incidence of os acromiale (based on imaging and arthroscopy) with concurrent rotator cuff tear and did not report surgical treatment or clinical outcomes and therefore were excluded. [31],[32] Three Level V evidence review studies were excluded. [2],[4],[33] Clinical follow-up of less than 24 months was found in two studies, [34],[35] and they were excluded. Five studies did not report the length of follow-up and were excluded. [36],[37],[38],[39],[40] One study did not report any demographic data of surgically treated patients and therefore was excluded. [41] Nine studies met all inclusion criteria and were analyzed further.
Subject inclusion criteria varied across studies, although, typically, were based on subacromial impingement symptoms (with or without the use of diagnostic subacromial lidocaine injection) and tenderness to palpation at a mobile/unstable os acromiale. Nomenclature of os acromiale types were based on the anterior fragment (e.g., an os acromiale between the pre- and mes-acromion was defined as a pre os acromiale; an os acromiale between the mesoacromion and metaacromion was defined as a meso-os acromiale; an os acromiale between the metaacromion and basiacromion was defined as a meta-os acromiale). Surgical techniques were described in detail within each study. For purposes of this review, os acromiale excision was defined as total/complete removal of the os acromiale, either arthroscopic or open. Acromioplasty was defined as incomplete removal of the os acromiale (either via open Neer acromioplasty or arthroscopic subacromial cutting-block acromioplasty). Fixation was defined as open or percutaneous internal placement of hardware fixing the os acromiale fragment to the more proximal scapula/acromion. Clinical assessment tools used postoperatively included the UCLA (University of California at Los Angeles) shoulder evaluation form, [42],[43],[44] PENN shoulder score, [45],[46] Constant score [47],[48] and ASES score (American Shoulder and Elbow Surgeons). [49] All but one study used postoperative X-rays. Two studies quantitatively reported isokinetic strength testing, [8],[48] while two more qualitatively reported postoperative strength. [42],[44]
A Z-test for two proportions (one-tailed, with assumption of acceptance of null hypothesis equivalent) was used to compare the proportions from two independent groups to test for significant differences between the acromioplasty and fixation groups (patient satisfaction), screw and K-wire fixation groups (rate of radiographic union) and requirement for removal of hardware following screw and K-wire fixation groups. Statistical analysis was performed using a free online statistical calculator. [50]
Results Top
Nine studies met the inclusion criteria (all Level IV evidence). [8],[9],[42],[44],[47],[48],[49],[10],[51] Two studies denied the presence of a financial conflict of interest (COI), [9],[48] while seven did not report the presence or absence of a COI. [8],[42],[44],[47],[49], [10],[11],[12],[13],[14],[15],[16],[17],[18],[19],[20],[21],[22],[23],[24],[25],[26],[27],[28],[29],[30],[31],[32],[33],[34],[35],[36],[37],[38],[39],[40],[41],[42],[43],[44],[45],[46],[47],[48],[49],[50],[51] One-hundred eighteen subjects were included (125 shoulders, seven bilateral cases). One-hundred fifteen subjects underwent surgical management of os acromiale (122 shoulders). Three subjects were managed nonoperatively (three shoulders). There were 82 males and 36 females. When reported (n=46), the right shoulder was involved 65% of the time (30/46) and, when reported (n=58), the dominant shoulder was involved 66% (38/58) of the time. The mean age of the subjects was 49±11 years (range, 18-73 years of age). The mean duration of the symptoms was 12±8.6 months (range, 2-36 months).
Meso-os acromiale was the most common type of os treated across all subjects in this review (94%). Internal fixation was the most common surgical technique (60%; 73/122), followed by excision (27%; 33/122) and acromioplasty (13%; 16/122). A “tension-band” technique with two parallel Kirschner wires and either stainless steel wire or suture in a cerclage or figure-of-eight technique was the most common fixation method (67%). Bone graft was used in 22 cases of fixation (30% of all fixation cases; 22/73; 16 iliac crest bone graft, six os graft). Rotator cuff repair was the most common concurrent surgical technique (59% of surgically treated shoulders; 72/122), followed by distal clavicle excision (25%; 31/122) and long-head biceps tenodesis (11%; 14/122). [Table 2] displays the distribution of the surgical techniques, [Table 3] displays the type of surgical fixation used and [Table 4] displays the concurrent surgical techniques used in addition to the surgical management of the os acromiale.
| Table 2: Surgical treatment distribution
Click here to view |
 |
Table 3: Types of surgical fixation and postoperative radiographic healing
Click here to view |
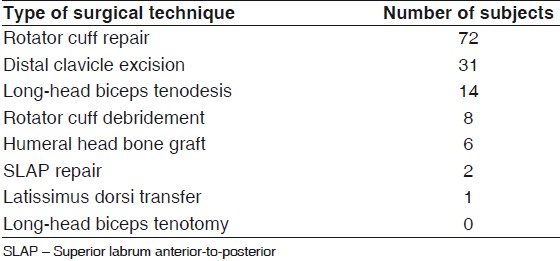 |
Table 4: Concurrent surgical techniques
Click here to view |
All surgical techniques resulted in improvement in clinical outcomes. [Table 5] displays the subject outcomes based on standardized clinical outcome measures. [Table 6] displays the range-of-motion outcomes. [Table 7] displays the individual study demographics.
| Table 5: Clinical outcomes
Click here to view |
| Table 6: Range-of-motion outcomes
Click here to view |
| Table 7: Individual study demographics
Click here to view |
Excision
Arthroscopic
No studies compared open and arthroscopic excision. Pagnani et al. performed the arthroscopic excision in 11 meso-os acromiales. [8] These patients, aged 18-25 years of age, were able to return to sport by 14 weeks postoperatively and demonstrated full isokinetic strength in abduction, internal rotation and external rotation versus the contralateral side. Wright et al. performed arthroscopic excision on 13 meso-os acromiales. [42] Although this cohort of patients was slightly older (mean, 36 years; range, 18-54 years), they all still demonstrated full anterior deltoid and rotator cuff strength by 6 months postoperatively, with 85% (11/13) patient satisfaction.
Open
Boehm et al.[48] and Warner et al.[9] performed open excision with deltoid re-attachment in nine os acromiales (four pre and five meso). In the former, patients (mean age, 56 years; range, 44-70 years) undergoing open os excision had equivalent Constant scores and patient satisfaction versus age- and gender-matched controls between those patients undergoing open Neer acromioplasty and fixation with either K-wire or cannulated screw tension-band constructs. Warner et al. (mean age, 57 years; range, 19-76 years) demonstrated a good outcome in a pre os excision and poor outcomes in both meso-os excisions (however, these were both following a failed internal fixation attempt).
Acromioplasty
Abboud et al. performed arthroscopic cutting-block (n=5) and open Neer (n=6) acromioplasty in 11 patients with a stable meso-os. [10] This group of patients was compared retrospectively with a group of eight patients undergoing open reduction and internal fixation with either K-wires (n=5) or cannulated screws (n=3). Although patient satisfaction (defined by improved pain, motion and strength) was greater in the acromioplasty group (7/11; 64%) versus the fixation group (3/8; 38%), the difference was not significant (Z=0.655; 95% confidence level). Boehm et al. also retrospectively compared patients undergoing open Neer acromioplasty versus internal fixation with K-wires. [48] Age- and gender-matched control comparison demonstrated equivalent Constant scores and patient satisfaction among the groups.
Fixation
Surgical fixation with cannulated screws led to a significantly greater rate of radiographic healing (96%; 23/24) versus fixation with Kirschner wires (63%; 31/49) (Z=2.735; 99.7% confidence level). The rate of radiographic healing correlated with significantly improved clinical outcome (UCLA score, ASES scores and patient satisfaction). Following screw fixation, Ryu et al.[44] demonstrated full strength and motion with normal UCLA score (35/35) in four of four patients (all radiographically united by 10-16 weeks postoperatively). Following screw fixation, Satterlee et al.[49] also demonstrated excellent ASES scores in six of six patients (all with radiographic union). Warner et al.[9] showed a significantly better union rate (86% versus 20%; 6/7 versus 1/5; Z=1.682; 95% confidence level) (mean 9-week time to union; range 7-20 weeks) following screw versus K-wire fixation. In this study, the union group demonstrated good clinical outcomes in six of the seven cases (86%), with the one patient experiencing a poor clinical outcome because of repeat rotator cuff tear rather than failure of fixation, while in the nonunion group, all patients demonstrated poor clinical outcome (five of five). Hertel et al.[47] demonstrated significantly greater Constant scores in patients with radiographic union versus nonunion (P=0.169). Ozbaydar et al.[51] demonstrated a significantly greater healing rate following screw versus K-wire fixation (four of four versus zero of two), with an overall improvement in the UCLA score from 11 to 28 (out of 35). Following K-wire fixation, Boehm et al.[48] showed a 68% union rate (15/22), although there was no difference between the union and nonunion groups with regard to Constant scores. Following both screw (n=3) and K-wire (n=5) fixation, Abboud et al.[10] showed a 100% union rate. Despite the latter, only three of the eight patients (38%; one screw and two K-wire) had a satisfactory clinical outcome (however, two of the five unsatisfied patients still had a good subjective rating). Requirement for removal of internal fixation hardware was significantly greater after Kirschner wire fixation cases (88%; 43/49) versus cannulated screw fixation cases (38%; 9/24) (Z=4.181; 100% confidence level).
Surgical complications
There were four cases of deep infection and two cases of superficial infection following surgical treatment of os acromiale. [48] One case of deep infection followed open excision, two cases followed open acromioplasty and one case followed open reduction and internal fixation. All these four cases required surgical incision and drainage. Two cases of superficial infection followed open reduction and internal fixation. These two cases responded to nonoperative, antibiotic management. There were no other complications following surgical intervention.
Discussion Top
The optimal surgical treatment for symptomatic os acromiale that had failed nonoperative management was unclear in the literature. The purpose of this review was to report and compare the clinical and radiographic outcomes following surgical management of symptomatic os acromiale. We hypothesized that (1) excision of pre os acromiale leads to improved clinical outcomes, while excision of meso- and meta-os acromiale fragments leads to poor clinical outcomes, (2) arthroscopic acromioplasty of stable os acromiale leads to improved clinical outcomes and (3) stable fixation of meso- and meta-os acromiale fragments leads to improved clinical outcomes.
This systematic review has shown that both arthroscopic and open excision of preacromiale and mesoacromiale lead to improved clinical outcomes, with full strength and motion and reduced pain. Both arthroscopic and open acromioplasty of mesoacromiale lead to improved patient satisfaction, with reduced pain and greater strength and motion. There is no significant difference in clinical outcome between acromioplasty and internal fixation. Fixation of mesoacromiale with cannulated screws versus K-wires leads to a significantly greater rate of radiographic healing and improved clinical outcome. Further, fixation with cannulated screws versus K-wires leads to a significantly reduced need for removal of internal fixation hardware.
Os acromiale may become symptomatic secondary to mobility at the site of failed fusion of ossification centers in the acromion. On attempted shoulder motion, deltoid firing pulls on the mobile fragment and may lead to dynamic subacromial impingement. Three general surgical techniques (open and arthroscopic) have been described to treat an os acromiale in a symptomatic patient that has failed nonsurgical treatments: excision, acromioplasty and internal fixation.
Fragment excision (either open or arthroscopic) may be able to significantly improve clinical outcomes with a meticulous surgical technique. Prior studies have demonstrated unacceptably poor outcomes with large os fragment excision and not repairing the deltoid origin. Neer et al. reviewed 30 consecutive patients that had radical acromionectomy and no deltoid repair. [30] All the patients had poor clinical results, with persistent pain and marked weakness, and over 25% had a serious wound complication. Further, deltoid scarring predictably led to extreme difficulty in the revision of the surgical situation. Bosley reviewed 35 consecutive patients that had total acromionectomy and meticulous deltoid repair to the remaining acromion. [29] Pain, motion, strength, function and patient satisfaction were excellent in 71% and good in 11% of the patients. Further, in four of five patients with the least satisfactory results, there was a chronic, massive rotator cuff tear confounding. Our review has demonstrated that both arthroscopic excision (that avoids disruption of the deltoid origin) and open excision with meticulous deltoid repair may significantly improve the clinical outcomes.
Acromioplasty of a stable os acromiale (either open or arthroscopic) may significantly improve the clinical outcomes, equivalent to that of internal fixation and excision groups and to that of age- and gender-matched controls. This technique works by reducing the dynamic bony impingement of the rotator cuff and subacromial bursa on the undersurface of the acromion. Arthroscopic acromioplasty should avoid disruption of the deltoid origin and open acromioplasty, just like open os excision, should attempt to carefully repair the deltoid attachment. Further, acromioplasty of unstable, mobile fragments may not lead to enough reduction in the dynamic impingement process and lead to poor clinical results.
Fixation of os acromiale significantly improves the clinical outcomes. Clinical outcome and radiographic healing of the unfused fragments appear to be related, regardless of type of fixation used. Healed fragments have a better clinical outcome than those that go on to nonunion. Low subject numbers and the lack of subject-level-specific data within this review preclude proof of correlation. Fixation with cannulated screws led to greater radiographic healing rates than fixation with K-wires, as did clinical outcome, and the reduced need for removal of hardware. The biomechanical composition of screws versus K-wires accounts for this. A screw is a more rigid, stiffer construct with threads and a thread depth that reduces/eliminates hardware pullout versus a K-wire, which is either smooth or with threads with a very small thread depth, more easily allowing for pullout. This may lead to skin complications due to prominent hardware and persistent pain.
The findings within this systematic review are inherently limited by the weaknesses within each study, specifically Level IV evidence. These studies were all retrospective in nature, with only one study performing matched control analysis. [48] Sources of selection bias within this review include different numbers of subjects within each surgical group analyzed and small numbers of subjects within each surgical group analyzed. The presence of concurrent surgical interventions (e.g. rotator cuff repair [open or arthroscopic], distal clavicle excision [open or arthroscopic], long head biceps tendon tenodesis, the use of autologous bone graft) is a source of performance bias, as are the minor technique variations within each surgical group analyzed.
Nearly all of the patients within this review had failed nonsurgical management measures prior to surgical intervention. Nevertheless, the lack of a nonoperative control group to compare the surgical techniques precludes the true outcomes of the surgical procedure itself. Assessment of clinical outcomes using validated outcome measures with measurement by independent observers is necessary to minimize detection bias. In this review, these parameters were either not performed or not reported in each of the studies. Further, heterogeneity of the assessment tools used in this review prevent accurate comparison, as do the definitions of patient satisfaction, excellent, good, fair, etc. The optimal assessment of an orthopedic disease treatment is by using a body-part-specific outcome tool and a general health outcome tool. This review lacked any general health outcome tools and only reported three shoulder-specific tools (UCLA, ASES and Constant) outcomes. Further, one study reported the use of the PENN outcome tool, but failed to actually report the subjects’ PENN scores. [10]
Conclusions Top
Surgical management of symptomatic os acromiale that has failed nonoperative measures may predictably lead to improved outcomes. Both arthroscopic and open excision of preacromiale and mesoacromiale lead to improved clinical outcomes, with full strength and motion and reduced pain. Both arthroscopic and open acromioplasty of mesoacromiale lead to improved patient satisfaction, with reduced pain and greater strength and motion. There is no significant difference in clinical outcome between acromioplasty and internal fixation. Fixation of mesoacromiale with cannulated screws versus K-wires leads to a significantly greater rate of radiographic healing and improved clinical outcome. Further, fixation with cannulated screws versus K-wires leads to a significantly reduced need for removal of internal fixation hardware.
References Top
1. McClure JG, Raney RB. Anomalies of the scapula. Clin Orthop Relat Res 1975;110:22-31. Back to cited text no. 1
[PUBMED]
2. Kurtz CA, Humble BJ, Rodosky MW, Sekiya JK. Symptomatic os acromiale. J Am Acad Orthop Surg 2006;14:12-19. Back to cited text no. 2
[PUBMED] [FULLTEXT]
3. Nicholson G, Goodman DA, Flatow EL, Bigliani LU. The acromion: Morphologic condition and age-related changes. A study of 420 scapulas. J Shoulder Elbow Surg 1996;5:1-11. Back to cited text no. 3
4. Sammarco VJ, Os acromiale: Frequency, anatomy, and clinical implications. J Bone Joint Surg Am 2000;82:394-400. Back to cited text no. 4
5. Liberson F. The value and limitation of the oblique view as compared with the ordinary anteroposterior exposure of the shoulder: A report of the use of the oblique view in 1,800 cases. Am J Roentgenol 1937;37:498-509. Back to cited text no. 5
6. Gruber W. Uber die arten der acromialknochen und accidentellen acromialgelenke. Arch. f. Anat. Physiol. u. wissensch. Med1863:373-87. Back to cited text no. 6
7. Becker F. Das Os acromiale und seine differentialdiagnose. Fortschr Geb Rontgenstr 1934;49:135-42. Back to cited text no. 7
8. Pagnani MJ, Mathis CE, Solman CG. Painful os acromiale (or unfused acromial apophysis) in athletes. J Shoulder Elbow Surg 2006;15:432-5. Back to cited text no. 8
[PUBMED] [FULLTEXT]
9. Warner JJ, Beim GM, Higgins L. The treatment of symptomatic os acromiale. J Bone Joint Surg Am 1998;80:1320-6. Back to cited text no. 9
[PUBMED] [FULLTEXT]
10. Abboud J, Silverberg D, Pepe M, Beredjiklian PK, Iannotti JP, Williams GR, et al. Surgical treatment of os acromiale with and without associated rotator cuff tears. J Shoulder Elbow Surg 2006;15:265-70. Back to cited text no. 10
11. Obremskey WT, Pappas N, Attallah-Wasif E, Tornetta P 3rd, Bhandari M. Levels of Evidence in Orthopaedic Journals. J Bone Joint Surg Am 2005;87:2632-8. Back to cited text no. 11
[PUBMED] [FULLTEXT]
12. Esenyel CZ, Demirhan M, Duygulu F. [Arthroscopic evaluation of the mobility of the meso-acromion]. Acta Orthop Traumatol Turc 2005;39:391-5. Back to cited text no. 12
[PUBMED] [FULLTEXT]
13. Burkhart SS. Os acromiale in a professional tennis player. Am J Sports Med 1992;20:483-4. Back to cited text no. 13
[PUBMED]
14. Demetropoulos CA, Kapadia NS, Herickhoff PK, Cosgarea AJ, McFarland EG. Surgical stabilization of os acromiale in a fast-pitch softball pitcher. Am J Sports Med 2006;34:1855-9. Back to cited text no. 14
15. Richards AM, Curtis MJ. Fracture of an os acromiale with associated rupture of the coracoclavicular ligaments. J Shoulder Elbow Surg 2008;17:e8-e11. Back to cited text no. 15
[PUBMED] [FULLTEXT]
16. Harnett PR, Ahrens PM, Gadikoppula SM. Rupture of the intra-articular portion of the long head of the biceps associated with a symptomatic os acromiale. Int J Shoulder Surg 2008;2:56-8. Back to cited text no. 16
[PUBMED] Medknow Journal
17. Sahajpal D, Strauss EJ, Ishak C, Keyes JM, Joseph G, Jazrawi LM. Surgical management of os acromiale – A case report and review of the literature. Bull NYU Hosp Jt Dis 2007;65:312-6. Back to cited text no. 17
[PUBMED] [FULLTEXT]
18. Davlin C, Fluker D. Bilateral os acromiale in a Division 1 basketball player. J Sports Sci Med 2003;2:175-9. Back to cited text no. 18
19. Carlson DW, Kim DH. Os acromiale. Am J Orthop (Belle Mead NJ) 2002;31:458. Back to cited text no. 19
[PUBMED]
20. Richman N, Curtis A, Hayman M. Acromion-splitting approach through an os acromiale for repair of a massive rotator cuff tear. Arthroscopy 1997;13:652-5. Back to cited text no. 20
[PUBMED]
21. Swain RA, Wilson FD, Harsha DM. The os acromiale: another cause of impingement. Med Sci Sports Exerc 1996;28:1459-62. Back to cited text no. 21
[PUBMED] [FULLTEXT]
22. Sterling JC, Meyers MC, Chesshir W, Calvo RD. Os acromiale in a baseball catcher. Med Sci Sports Exerc 1995;27:795-9. Back to cited text no. 22
[PUBMED]
23. Jerosch J, Hepp R, Castro WH. An unfused acromial epiphysis – A reason for chronic shoulder pain. Acta Orthop Belg 1991;57:309-12. Back to cited text no. 23
[PUBMED]
24. Sassmannshausen G, Wilson TC, Mair SD. Operative stabilization of an unstable os acromiale in an adolescent football player. Orthopedics 2003;26:509-11. Back to cited text no. 24
[PUBMED]
25. Ouellette H, Thomas BJ, Kassarjian A, Fritz B, Tétreault P, Palmer WE, et al. Re-examining the association of os acromiale with supraspinatus and infraspinatus tears. Skeletal Radiol 2007;36:835-9. Back to cited text no. 25
26. Boehm TD, Kenn W, Matzer M, Gohlke F. Ultrasonographic appearance of os acromiale. Ultraschall Med 2003;24:180-3. Back to cited text no. 26
[PUBMED] [FULLTEXT]
27. Granieri GF, Bacarini L. A little-known cause of painful shoulder: Os acromiale. Eur Radiol 1998;8:130-3. Back to cited text no. 27
[PUBMED] [FULLTEXT]
28. Lee DH, Lee KH, Lopez-Ben R, Bradley EL. The double-density sign: A radiographic finding suggestive of an os acromiale. J Bone Joint Surg Am 2004;86:2666-70. Back to cited text no. 28
[PUBMED] [FULLTEXT]
29. Bosley RC. Total acromionectomy. A twenty-year review. J Bone Joint Surg Am 1991;73:961-8. Back to cited text no. 29
[PUBMED]
30. Neer CS, Marberry TA. On the disadvantages of radical acromionectomy. J Bone Joint Surg Am 1981;63:416-9. Back to cited text no. 30
31. Mudge MK, Wood VE, Frykman GK. Rotator cuff tears associated with os acromiale. J Bone Joint Surg Am 1984;66:427-9. Back to cited text no. 31
[PUBMED]
32. Boehm TD, Rolf O, Martetschlaeger F, Kenn W, Gohlke F. Rotator cuff tears associated with os acromiale. Acta Orthop 2005;76:241-4. Back to cited text no. 32
[PUBMED]
33. Ortiguera CJ, Buss DD. Surgical management of the symptomatic os acromiale. J Shoulder Elbow Surg 2002;11:521-8. Back to cited text no. 33
[PUBMED] [FULLTEXT]
34. Hutchinson MR, Veenstra MA. Arthroscopic decompression of shoulder impingement secondary to os acromiale. Arthroscopy 1993;9:28-32. Back to cited text no. 34
[PUBMED]
35. Peckett WR, Gunther SB, Harper GD, Hughes JS, Sonnabend DH. Internal fixation of symptomatic os acromiale: A series of twenty-six cases. J Shoulder Elbow Surg 2004;13:381-5. Back to cited text no. 35
[PUBMED] [FULLTEXT]
36. Bigliani LU, Norris TR, Fischer J. The relationship between the unfused acromial epiphysis and subacromial impingement lesions. Orthop Trans 1983;7:138. Back to cited text no. 36
37. Osaki M, Kondo M. Rotator cuff tear associated with os acromiale, a report of six cases. J Shoulder Elbow Surg 1993;2:S35. Back to cited text no. 37
38. Norris T. The unfused acromial epiphysis and its relationship to impingement. Orthop Trans 1983;7:505-6. Back to cited text no. 38
39. Armengol J, Brittis D, Pollock RG, Flatow EL, Self EB, Bigliani LU. The association of an unfused acromial epiphysis with tears of the rotator cuff: a review of 42 cases. J Shoulder Elbow Surg 1994;3:s14. Back to cited text no. 39
40. Armengol J, Brittis D, Pollock RG, Flatow EL, Self EB, Bigliani LU. The surgical treatment of an unfused acromial epiphysis in association with a tear of the rotator cuff: A review of 41 cases. J Shoulder Elbow Surg 1993;2:S24. Back to cited text no. 40
41. Edelson JG, Zuckerman J, Hershkovitz I. Os acromiale: Anatomy and surgical implications. J Bone Joint Surg Br 1993;75:551-5. Back to cited text no. 41
[PUBMED] [FULLTEXT]
42. Wright RW, Heller MA, Quick DC, Buss DD. Arthroscopic decompression for impingement syndrome secondary to unstable os acromiale. Arthroscopy 2000;16:595-9. Back to cited text no. 42
[PUBMED] [FULLTEXT]
43. Ellman H, Hanker G, Bayer M. Repair of the rotator cuff. End-result study of factors influencing reconstruction. J Bone Joint Surg Am 1986;68:1136-44. Back to cited text no. 43
[PUBMED]
44. Ryu RK, Fan RS, Dunbar WH 5th. The treatment of symptomatic os acromiale. Orthopedics 1999;22:325-8. Back to cited text no. 44
[PUBMED]
45. Leggin BG, Michener LA, Shaffer MA, Brenneman SK, Iannotti JP, Williams GR Jr. The Penn Shoulder Score: Reliability and Validity. J Orthop Sports Phys Ther 2006;36:138-51. Back to cited text no. 45
[PUBMED]
46. Leggin BG, Neuman RM, Shaffer MA, Iannotti JP, Williams GR, Brenneman SK. Reliability and validity of a shoulder outcome scoring system. J Orthop Sports Phys Ther 1996;23:65. Back to cited text no. 46
47. Hertel R, Windisch W, Schuster A, Ballmer FT. Transacromial approach to obtain fusion of unstable os acromiale. J Shoulder Elbow Surg 1998;7:606-9. Back to cited text no. 47
[PUBMED]
48. Boehm TD, Matzer M, Brazda D, Gohlke FE. Os acromiale associated with tear of the rotator cuff treated operatively. J Bone Joint Surg Br 2003;85:545-9. Back to cited text no. 48
[PUBMED] [FULLTEXT]
49. Satterlee CC. Successful osteosynthesis of an unstable mesoacromion in 6 shoulders: A new technique. J Shoulder Elbow Surg 1999;8:125-9. Back to cited text no. 49
[PUBMED]
50. Inc., D.R., Z-test for two proportions. 2010. Back to cited text no. 50
51. Ozbaydar MU, Keris I, Altun M, Yalaman O. Results of the surgical treatment for symptomatic mesoacromion. Acta Orthop Traumatol Turc 2006;40:123-9. Back to cited text no. 51
Figures
[Figure 1]
Tables
[Table 1], [Table 2], [Table 3], [Table 4], [Table 5], [Table 6], [Table 7]
